290:, which gives the clinician an approximation of the infant's cardiovascular and neurologic condition at birth. A score of 7–10 at 5 minutes is normal, a score of 4 to 6 at 5 minutes is intermediate, and a score of 0-3 is considered low. It is important to understand that an Apgar score is not a diagnosis, it is merely a clinical finding. If a newborns score is 0–3, then resuscitation efforts are initiated.
294:
405:
published articles and found that high-income countries have a mortality rate as high as 10% while low-income countries have a mortality rate as high as 28%. One major factor that improved survival was how quickly medical responders were able to intervene, noting that the first minutes are critical.
108:
Up to 10% of infants are born requiring assistance to begin breathing. After assistance, many of these infants begin to breath on their own and are healthy. Breathing problems at birth is a high priority emergency and interventions such as breathing support and resuscitation is sometimes required.
601:
Wyckoff, Myra H.; Wyllie, Jonathan; Aziz, Khalid; de
Almeida, Maria Fernanda; Fabres, Jorge; Fawke, Joe; Guinsburg, Ruth; Hosono, Shigeharu; Isayama, Tetsuya; Kapadia, Vishal S.; Kim, Han-Suk; Liley, Helen G.; McKinlay, Christopher J.D.; Mildenhall, Lindsay; Perlman, Jeffrey M. (2020-10-20).
29:
215:, and others. The course is broken down into 11 sections and a final skills assessment. There are currently 4 million healthcare providers that are certified. It is estimated that 200,000 healthcare providers take this course every year.
422:
infants have little or no difference in risk of death or neurodevelopment disability when higher concentrations of oxygen are used compared to lower concentrations but the evidence from clinical trials is still relatively uncertain.
417:
after asphyxia. Clinical trial evidence suggests that resuscitation using air probably reduces the risk of death and the 2010 ILCOR guidelines recommend the use of normal air rather than 100% oxygen. Another study showed that
1133:
396:
Apgar score of 5.9, which is considered intermediate. More data is needed to understand outcomes for more severe patients. Outcomes after resuscitation for neonates vary widely based on many factors. One study in
256:(ILCOR) published its 4th and most recent recommendations for newborn life support. The committee reviewed 8 major topics, including anticipation and preparation, initial assessment and intervention,
93:, and in severe cases chest compressions, medical personnel certified in neonatal resuscitation can often stimulate neonates to begin breathing on their own, with attendant normalization of
438:
in order to classify the severity of brain damage. However, one study found that there was no significant correlation between MRI findings and developmental delay up to 2 years of life.
100:
Face masks that cover the infant's mouth and nose are often used in the resuscitation procedures. Nasal prongs/tubes/masks and laryngeal mask airway devices are also sometimes used.
245:
with 100% oxygen, but there has since the 1980s increasingly been debated whether newborn infants with asphyxia should be resuscitated with 100% oxygen or normal air, and notably
695:; Rootwelt, T; Aalen, O (1998). "Resuscitation of asphyxiated newborn infants with room air or oxygen: an international controlled trial: the Resair 2 study".
604:"Neonatal Life Support: 2020 International Consensus on Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Science With Treatment Recommendations"
392:
Most neonatal deaths (roughly 75%) after resuscitation occur within the first week, but the vast majority occur within 24 hours. This statistic is based on a
316:
Guidelines for neonatal resuscitation are assessed annually and are developed in collaboration with multiple organizations of numerous experts, including the
370:
For uncomplicated term or preterm infants, delayed cord clamping is standard so that the child can immediately be placed in the mothers arms to be evaluated.
852:"Practice and outcomes of neonatal resuscitation for newborns with birth asphyxia at Kakamega County General Hospital, Kenya: a direct observation study"
732:
Davis, PG; Tan, A; O'Donnell, CPF; Schulze, A (2004). "Resuscitation of newborn infants with 100% oxygen or air: a systematic review and meta-analysis".
199:, this course has been revised several times and is currently offered to anyone who participates in neonatal resuscitation including but not limited to:
128:
with a 'manual ventilation device' to provide breathing support. Examples of manual ventilation devices include a self-inflating bag or a T-piece.
253:
234:
802:
345:(PPV) for either ineffective respirations or bradycardia should not also receive initially sustained inflations greater than 5 seconds.
1016:"Lower versus higher oxygen concentrations titrated to target oxygen saturations during resuscitation of preterm infants at birth"
915:"Hydrogen peroxide production in leukocytes during cerebral hypoxia and reoxygenation with 100% or 21% oxygen in newborn piglets"
777:
455:
152:. Depending on how quickly and successfully the infant is resuscitated, hypoxic damage can occur to most of the infant's organs (
535:
Ni
Chathasaigh, Caitriona M; Davis, Peter G; O'Donnell, Colm PF; McCarthy, Lisa K (2023-10-03). Cochrane Neonatal Group (ed.).
1065:"Neonatal hypoxic encephalopathy: Correlation between post-cooling brain MRI findings and 2 years neurodevelopmental outcome"
1063:
Rusli, Emilia
Rosniza Mohammed; Ismail, Juriza; Wei, Wong Saw; Ishak, Shareena; Jaafar, Rohana; Zaki, Faizah Mohd (2019).
434:. This is done in order to minimize brain swelling. After cooling is achieved, an MRI is obtained roughly 1 week after
221:(PALS) - This program is more general to all pediatric patients, but does provide some neonatal resuscitation training.
651:
366:
While some guidelines do tend to change, certain elements of neonatal resuscitation have persisted. These include:
359:
431:
218:
317:
196:
192:
185:
89:. Many of the infants who require this support to start breathing well on their own after assistance. Through
1128:
342:
306:
277:
125:
302:
212:
136:
About a quarter of all neonatal deaths globally are caused by birth asphyxia. This dangerous condition of
850:
Shikuku, Duncan N.; Milimo, Benson; Ayebare, Elizabeth; Gisore, Peter; Nalwadda, Gorrette (2018-05-15).
261:
90:
352:
is administered if the heart rate does not increase to 60 beats per minute after ventilation and
173:
124:
with a heart rate lower than 100 beats per minute after birth are recommended to be administered
603:
242:
265:
208:
697:
427:
145:
323:
In 2020, the ILCOR recommended the following changes to current resuscitation guidelines:
8:
910:
692:
409:
It has been demonstrated that high concentrations of oxygen lead to generation of oxygen
246:
113:
74:
668:
561:
1099:
1064:
1040:
1015:
1014:
Lui, K; Jones, LJ; Foster, JP; Davis, PG; Ching, SK; Oei, JL; Osborn, DA (4 May 2018).
982:
957:
919:
886:
851:
759:
507:
480:
414:
353:
269:
747:
536:
1104:
1086:
1045:
987:
938:
933:
914:
891:
873:
832:
824:
751:
714:
647:
625:
566:
512:
435:
137:
36:
763:
376:
Monitoring of heart rate is the best indicator of response to resuscitation efforts.
309:(PPV), updated timings on ventilation assistance rates, and some differences in the
1094:
1076:
1035:
1031:
1027:
977:
973:
969:
928:
881:
863:
814:
743:
706:
615:
556:
552:
548:
502:
492:
620:
332:
310:
184:
The most widely known training/certification for neonatal resuscitation is the
141:
868:
497:
1122:
1090:
877:
828:
629:
419:
410:
380:
328:
239:
Consensus on science and treatment recommendations for neonatal resuscitation
165:
1081:
819:
1108:
1049:
991:
942:
895:
836:
755:
570:
516:
718:
710:
56:
1134:
Respiratory and cardiovascular disorders specific to the perinatal period
402:
349:
287:
121:
534:
801:
Boldingh, Anne Marthe; Solevåg, Anne Lee; Nakstad, Britt (2018-05-28).
734:
669:"Who Can Benefit from a Neonatal Resuscitation Program? | NRP Training"
335:
257:
149:
94:
273:
204:
82:
393:
169:
301:
Neonatal resuscitation guidelines closely resemble those of the
430:
to place neonates on a cooling blanket for 72 hours to achieve
398:
241:. Traditionally, newborn children have been resuscitated using
200:
78:
956:
Tan, A; Schulze, A; O'Donnell, CP; Davis, PG (18 April 2005).
293:
161:
153:
117:
86:
28:
955:
908:
731:
362:
should be the primary vascular access route during delivery.
803:"Outcomes following neonatal cardiopulmonary resuscitation"
600:
479:
Johnson, Peter A.; Schmölzer, Georg M. (23 February 2020).
338:
for newborns with clear or meconium-stained amniotic fluid.
157:
849:
958:"Air versus oxygen for resuscitation of infants at birth"
305:
The main differences in training include an emphasis on
286:
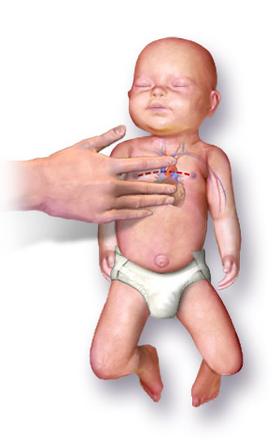
Initial evaluation of a newborn is done by obtaining an
85:, putting them at risk of irreversible organ injury and
172:). One serious complication is a brain injury known as
800:
691:
481:"Heart Rate Assessment during Neonatal Resuscitation"
1062:
1013:
49:10% of newborns who do not readily begin breathing
1120:
478:
254:International Liaison Committee on Resuscitation
235:International Liaison Committee on Resuscitation
249:has been a major advocate of using normal air.
1069:The Indian Journal of Radiology & Imaging
537:"Nasal interfaces for neonatal resuscitation"
179:
1004:ILCOR Neonatal Resuscitation Guidelines 2010
140:may begin before birth. For example, if the
1020:The Cochrane Database of Systematic Reviews
962:The Cochrane Database of Systematic Reviews
646:. Geneva: World Health Organization. 2012.
228:
77:focused on supporting approximately 10% of
383:if response to chest compressions is poor.
303:pediatric basic and advanced life support.
27:
1098:
1080:
1039:
981:
932:
885:
867:
818:
666:
644:Guidelines on basic newborn resuscitation
619:
560:
506:
496:
373:Supplemental oxygen is used judiciously.
292:
272:support, drug and fluid administration,
174:neonatal hypoxic-ischemic encephalopathy
541:Cochrane Database of Systematic Reviews
1121:
807:Tidsskrift for den Norske Legeforening
778:"Neonatal Resuscitation - Pediatrics"
456:"Neonatal Resuscitation - Pediatrics"
909:Kutzsche, S; Ilves, P; Kirkeby, OJ;
596:
594:
592:
590:
588:
586:
584:
582:
580:
530:
528:
526:
379:Epinephrine should be administered
144:, which supplies oxygen throughout
120:(suspension of breathing), or have
13:
843:
782:Merck Manuals Professional Edition
460:Merck Manuals Professional Edition
14:
1145:
667:Heartbeat, Project (2019-03-13).
577:
523:
260:monitoring and feedback devices,
934:10.1203/00006450-200106000-00020
360:umbilical venous catheterization
148:, is compressed or tears during
131:
1056:
1007:
998:
949:
902:
794:
297:Apgar score for newborn infants
280:, and post-resuscitation care.
219:Pediatric Advanced Life Support
1032:10.1002/14651858.CD010239.pub2
974:10.1002/14651858.CD002273.pub3
770:
725:
685:
660:
636:
553:10.1002/14651858.CD009102.pub2
472:
448:
318:American Academy of Pediatrics
197:American Academy of Pediatrics
193:Neonatal Resuscitation Program
186:Neonatal Resuscitation Program
16:An emergency medical procedure
1:
748:10.1016/S0140-6736(04)17189-4
441:
343:Positive Pressure Ventilation
307:positive pressure ventilation
126:positive pressure ventilation
621:10.1161/CIR.0000000000000895
213:Certified Nursing Assistants
7:
387:
10:
1150:
180:Training and certification
869:10.1186/s12887-018-1127-6
498:10.3390/healthcare8010043
81:who do not readily begin
53:
45:
35:
26:
21:
229:Resuscitation guidelines
91:positive airway pressure
1082:10.4103/ijri.IJRI_62_19
820:10.4045/tidsskr.17.0358
413:, which have a role in
116:', show signs of being
103:
67:Neonatal resuscitation,
298:
243:mechanical ventilation
237:(ILCOR) has published
209:Respiratory Therapists
71:newborn resuscitation,
22:Neonatal resuscitation
711:10.1542/peds.102.1.e1
426:Currently, it is the
341:Newborns who receive
296:
112:All infants who are '
1129:Respiratory diseases
436:hypoxic brain injury
356:have been optimized.
224:On-the-job training.
742:(9442): 1329–1333.
313:chain of survival.
247:Ola Didrik Saugstad
75:emergency procedure
920:Pediatric Research
432:total body cooling
415:reperfusion injury
354:chest compressions
299:
138:oxygen deprivation
673:Project Heartbeat
195:- Started by the
146:fetal development
64:
63:
1141:
1113:
1112:
1102:
1084:
1060:
1054:
1053:
1043:
1011:
1005:
1002:
996:
995:
985:
953:
947:
946:
936:
906:
900:
899:
889:
871:
847:
841:
840:
822:
798:
792:
791:
789:
788:
774:
768:
767:
729:
723:
722:
689:
683:
682:
680:
679:
664:
658:
657:
640:
634:
633:
623:
598:
575:
574:
564:
532:
521:
520:
510:
500:
476:
470:
469:
467:
466:
452:
79:newborn children
57:edit on Wikidata
31:
19:
18:
1149:
1148:
1144:
1143:
1142:
1140:
1139:
1138:
1119:
1118:
1117:
1116:
1061:
1057:
1026:(5): CD010239.
1012:
1008:
1003:
999:
968:(2): CD002273.
954:
950:
907:
903:
848:
844:
799:
795:
786:
784:
776:
775:
771:
730:
726:
690:
686:
677:
675:
665:
661:
654:
642:
641:
637:
599:
578:
533:
524:
477:
473:
464:
462:
454:
453:
449:
444:
390:
283:
274:prognostication
231:
182:
134:
106:
60:
17:
12:
11:
5:
1147:
1137:
1136:
1131:
1115:
1114:
1075:(4): 350–355.
1055:
1006:
997:
948:
927:(6): 834–842.
901:
856:BMC Pediatrics
842:
793:
769:
724:
684:
659:
652:
635:
614:(16_suppl_1).
576:
522:
471:
446:
445:
443:
440:
389:
386:
385:
384:
377:
374:
371:
364:
363:
357:
346:
339:
333:nasopharyngeal
311:cardiac arrest
230:
227:
226:
225:
222:
216:
181:
178:
142:umbilical cord
133:
130:
105:
102:
69:also known as
62:
61:
54:
51:
50:
47:
43:
42:
39:
33:
32:
24:
23:
15:
9:
6:
4:
3:
2:
1146:
1135:
1132:
1130:
1127:
1126:
1124:
1110:
1106:
1101:
1096:
1092:
1088:
1083:
1078:
1074:
1070:
1066:
1059:
1051:
1047:
1042:
1037:
1033:
1029:
1025:
1021:
1017:
1010:
1001:
993:
989:
984:
979:
975:
971:
967:
963:
959:
952:
944:
940:
935:
930:
926:
922:
921:
916:
912:
905:
897:
893:
888:
883:
879:
875:
870:
865:
861:
857:
853:
846:
838:
834:
830:
826:
821:
816:
812:
808:
804:
797:
783:
779:
773:
765:
761:
757:
753:
749:
745:
741:
737:
736:
728:
720:
716:
712:
708:
704:
700:
699:
694:
688:
674:
670:
663:
655:
653:9789241503693
649:
645:
639:
631:
627:
622:
617:
613:
609:
605:
597:
595:
593:
591:
589:
587:
585:
583:
581:
572:
568:
563:
558:
554:
550:
546:
542:
538:
531:
529:
527:
518:
514:
509:
504:
499:
494:
490:
486:
482:
475:
461:
457:
451:
447:
439:
437:
433:
429:
428:gold standard
424:
421:
416:
412:
411:free radicals
407:
404:
403:peer-reviewed
400:
395:
382:
381:intravenously
378:
375:
372:
369:
368:
367:
361:
358:
355:
351:
347:
344:
340:
337:
334:
330:
329:oropharyngeal
326:
325:
324:
321:
319:
314:
312:
308:
304:
295:
291:
289:
284:
281:
279:
275:
271:
267:
263:
259:
255:
252:In 2020, the
250:
248:
244:
240:
236:
223:
220:
217:
214:
210:
206:
202:
198:
194:
191:
190:
189:
187:
177:
175:
171:
167:
163:
159:
155:
151:
147:
143:
139:
132:Complications
129:
127:
123:
119:
115:
110:
101:
98:
96:
92:
88:
84:
80:
76:
72:
68:
58:
52:
48:
44:
40:
38:
34:
30:
25:
20:
1072:
1068:
1058:
1023:
1019:
1009:
1000:
965:
961:
951:
924:
918:
911:Saugstad, OD
904:
859:
855:
845:
810:
806:
796:
785:. Retrieved
781:
772:
739:
733:
727:
702:
696:
693:Saugstad, OD
687:
676:. Retrieved
672:
662:
643:
638:
611:
607:
544:
540:
488:
484:
474:
463:. Retrieved
459:
450:
425:
408:
401:analyzed 15
391:
365:
348:Intravenous
322:
315:
300:
285:
282:
251:
238:
232:
183:
135:
111:
107:
99:
70:
66:
65:
608:Circulation
350:epinephrine
288:Apgar score
270:circulatory
266:oxygenation
262:ventilation
258:physiologic
122:bradycardia
41:neonatology
1123:Categories
862:(1): 167.
787:2021-11-09
735:The Lancet
698:Pediatrics
678:2021-11-11
485:Healthcare
465:2019-11-13
442:References
336:suctioning
205:Physicians
95:heart rate
1091:0971-3026
878:1471-2431
829:0029-2001
705:(1): e1.
630:0009-7322
491:(1): 43.
83:breathing
46:Frequency
37:Specialty
1109:31949335
1050:29726010
992:15846632
943:11385146
913:(2001).
896:29764391
837:29808658
764:24825982
756:15474135
571:37787113
562:10546484
517:32102255
388:Outcomes
327:Ceasing
150:delivery
1100:6958878
1041:6494481
983:7017642
887:5953400
719:9651453
508:7151423
420:preterm
320:(AAP).
276:during
188:(NRP).
170:kidneys
118:apnoeic
114:gasping
1107:
1097:
1089:
1048:
1038:
990:
980:
941:
894:
884:
876:
835:
827:
762:
754:
717:
650:
628:
569:
559:
547:(10).
515:
505:
399:Norway
201:Nurses
73:is an
813:(9).
760:S2CID
162:liver
158:lungs
154:heart
87:death
55:[
1105:PMID
1087:ISSN
1046:PMID
988:PMID
966:2005
939:PMID
892:PMID
874:ISSN
833:PMID
825:ISSN
752:PMID
715:PMID
648:ISBN
626:ISSN
567:PMID
545:2023
513:PMID
394:mean
331:and
264:and
233:The
104:Uses
1095:PMC
1077:doi
1036:PMC
1028:doi
978:PMC
970:doi
929:doi
882:PMC
864:doi
815:doi
811:138
744:doi
740:364
707:doi
703:102
616:doi
612:142
557:PMC
549:doi
503:PMC
493:doi
278:CPR
166:gut
1125::
1103:.
1093:.
1085:.
1073:29
1071:.
1067:.
1044:.
1034:.
1022:.
1018:.
986:.
976:.
964:.
960:.
937:.
925:49
923:.
917:.
890:.
880:.
872:.
860:18
858:.
854:.
831:.
823:.
809:.
805:.
780:.
758:.
750:.
738:.
713:.
701:.
671:.
624:.
610:.
606:.
579:^
565:.
555:.
543:.
539:.
525:^
511:.
501:.
487:.
483:.
458:.
268:,
211:,
207:,
203:,
176:.
168:,
164:,
160:,
156:,
97:.
1111:.
1079::
1052:.
1030::
1024:5
994:.
972::
945:.
931::
898:.
866::
839:.
817::
790:.
766:.
746::
721:.
709::
681:.
656:.
632:.
618::
573:.
551::
519:.
495::
489:8
468:.
59:]
Text is available under the Creative Commons Attribution-ShareAlike License. Additional terms may apply.